Penn Study Identifies New Trigger for Breast Cancer Metastasis
For years, scientists have observed that tumor cells from certain breast cancer patients with aggressive forms of the disease contained low levels of mitochondrial DNA. But, until recently, no one was able to explain how this characteristic influenced disease progression.
Now, University of Pennsylvania researchers have revealed how a reduction in mitochondrial DNA content leads human breast cancer cells to take on aggressive, metastatic properties. The work, published in the journal Oncogene, breaks new ground in understanding why some cancers progress and spread faster than others and may offer clinicians a biomarker that would distinguish patients with particularly aggressive forms of disease, helping personalize treatment approaches.
The study was led by the Penn School of Veterinary Medicine’s Manti Guha, a senior research investigator, and Narayan Avadhani, Harriet Ellison Woodward Professor of Biochemistry in the Department of Animal Biology. Additional Penn Vet collaborators included Satish Srinivasan, Gordon Ruthel, Anna K. Kashina and Thomas Van Winkle. They teamed with Russ P. Carstens of Penn’s Perelman School of Medicine and Arnulfo Mendoza and Chand Khanna of the National Cancer Institute.
Mitochondria, the “powerhouses” of mammalian cells, are also a signaling hub. They are heavily involved in cellular metabolism as well as in apoptosis, the process of programmed cell death by which potentially cancerous cells can be killed before they multiply and spread. In addition, mitochondria contain their own genomes, which code for specific proteins and are expressed in coordination with nuclear DNA to regulate the provision of energy to cells.
In mammals, each cell contains between 100 and 1,000 copies of mitochondrial DNA, but previous research had found that as many as 80 percent of people with breast cancer have low mitochondrial DNA, or mtDNA, content.
To gain an understanding of the mechanism that connects low mtDNA levels with a cellular change that leads to cancer and metastasis, Guha, Avadhani and their colleagues set up two systems by which they could purposefully reduce the amount of mtDNA in a cell. One used a chemical to deplete the DNA content, and another altered mtDNA levels genetically. They compared normal, non-cancer-forming human breast tissue cells with cancerous breast cells using both of these treatments, contrasting them with cells with unmanipulated mtDNA.
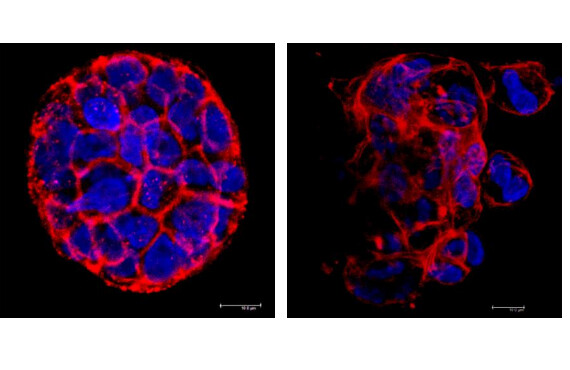
The differences between cells with unmodified and reduced mtDNA levels were striking, the researchers found. The cells in which mtDNA was reduced had altered metabolism and their structure appeared disorganized, more like that of a metastatic cancer cell. Even the non-tumor-forming breast cells became invasive and more closely resembled cancer cells. Significantly, cells with reduced mtDNA became self-renewing and expressed specific cell surface markers characteristic of breast cancer stem cells.
“Reducing mitochondrial DNA makes mammary cells look like cancerous stem cells,” Avadhani said. “These cells acquire the characteristics of stem cells, that is the ability to propagate and migrate, in order to begin the process of metastasis and move to distal sites in the body.”
“Most patients who had low copy numbers of mitochondrial DNA have a poor disease prognosis,” Guha said. “We’ve shown a causal role for this mitochondrial defect and identified a candidate biomarker for aggressive forms of the disease. In the future, mtDNA and the factors involved in mitochondrial signaling may serve as markers of metastatic potential and novel points for therapeutic intervention of cancer stem cells. Since the specific inducers of cancer stem cells, which are key drivers of metastasis, remain elusive, our current findings are a significant advancement in this area.”
No two breast cancers are exactly alike, so having a way to recognize patients who are at high-risk for developing particularly invasive and rapidly metastasizing cancers could help physicians customize treatments. In addition, researchers are currently filling in the unknown components of the signaling pathway linking a cell’s mitochondrial DNA levels and its involvement in metastatic disease.
As a next step, Guha, Avadhani and colleagues plan to extend this study to in vivo mouse models and will also investigate these mechanisms in tumor samples from human breast cancer patients.
This study was funded by the National Institutes of Health and the Harriet Ellison Woodward Trust.