Penn Oral and Maxillofacial Surgeon Driven by Desire to ‘Make Someone Whole Again’
In his office at the University of Pennsylvania, oral and maxillofacial surgeon Rabie Shanti sits at his computer, clicking through photos of patients he’s operated on.
He pulls up an image of a mouth open wide, tongue extended.
“This is a recent case,” he says, pointing to one side of the tongue that looks slightly different from the other. “This is forearm skin with an artery and vein taken from the arm. That surgery was done the same day the patient had their tongue cancer resected. We used those tissues and vessels to reconstruct the tongue to allow this patient to maintain their ability to eat and speak after having almost half of their tongue removed.”
Those familiar with grafting surgery may understand that, after a burn, for example, surgeons can take portions of skin from one part of the body to replace skin lost from another area. But what Shanti is describing is something even more mind-bending. He reconstructs tongues, as well as other portions of the oral cavity, using tissues and bone harvested from other parts of the patient’s own body.
The work is remarkable, but taxing for the patient. So when he’s not busy in the clinic, Shanti, who joined Penn’s School of Dental Medicine as an assistant professor last year, is devoting energy in the lab to better understand what drives oral cancers and to design new structures that will more effectively replace the tissues his patients lose during surgery, whether due to cancerous or benign tumors, trauma or inflammatory conditions.
“I think that I was always fascinated with the idea of putting something back together,” says Shanti, who also holds an appointment as assistant professor in Penn’s Perelman School of Medicine. “Most of what is done in dentistry is really reconstructive, whether it’s rebuilding the tooth surface or part of the jaw.”
When Shanti was a college student at Florida Atlantic University, he became interested in pursuing dental medicine as a career, though being a surgeon was not on his radar.
“At that time, aside from having braces, I had no deep experience with dentistry,” he says. “I thought I wanted to be an orthodontist. I didn’t know what an oral and maxillofacial surgeon was until I was in dental school.”
He attended dental school at Harvard University, pausing his studies to spend two years as a Howard Hughes Medical Institute research scholar working in an orthopedics laboratory at the National Institutes of Health’s National Institute for Arthritis and Musculoskeletal and Skin Diseases. The lab was headed by Rocky Tuan, who is now at the University of Pittsburgh. At the NIAMS, Shanti delved into tissue engineering, focusing on designing new materials to help regrow muscle and bone.
“I quickly noticed that my research interests were fueled by my clinical interests, and one area that really interested me was reconstructive surgery of the jaw and tongue, particularly reconstruction for pathology,” he says. “Seeing someone who had a benign tumor or cancer that involved their upper or lower jaw bone, and now they’ve lost that part of their body, but being able to make someone whole again, that really drew me in.”
After completing his dental degree, Shanti went on to pursue his residency in oral and maxillofacial surgery at Rutgers University, an experience he likens to “being a kid in a candy store,” enticed by all the possible areas in which to focus. He earned his M.D. at Rutgers along the way. He then went on to Louisiana State University for a two-year fellowship, pursuing research and bolstering his experience in reconstructive microsurgery, which involves taking tissues and blood vessels from one part of the body and connecting them to another part of the body to make it a living tissue. Shanti left LSU for Penn in 2016.
Through much of his training and still today, Shanti has pursued research in an area that sparked his interest early on in dental school: ameloblastoma, a rare tumor of the jaw, affecting 1 in 2 million people. This tumor type is resistant to most forms of treatment, leaving patients with surgery as the only viable option. These procedures often result in the loss of large portions of the lower or upper jaw.
Shanti’s investigations have examined the role of mesenchymal stem cells, which dwell in the bone marrow, in supporting ameloblastoma tumors. Working with his research mentor, Anh Le, the Norman Vine Endowed Professor of Oral Rehabilitation and chair of the Department of Oral and Maxillofacial Surgery/Pharmacology at Penn Dental Medicine, Shanti has looked for ways to disrupt the communication between these stem cells and tumor cells as a way of possible preventing their aggressive growth.
A second research interest for Shanti is tissue engineering, specifically to improve tongue reconstructions. The tongue can be affected by invasive squamous cell carcinoma, and to treat it can involve removing large portions of tissue. Shanti works closely with Le in her lab at Penn Dental Medicine toward engineering constructs that could help a patient regrow tissue rather than using tissue taken from another body part.
“I think we’re on the cusp with tissue engineering and using engineered stem-cell-based constructs to reconstruct tissues of the head and neck,” says Shanti. “I think that’s going to be a really significant advancement in reconstructive surgery that I hope to be a part of during my career and lifetime.”
In the clinic, Shanti alternates time seeing patients at the Hospital of the University Pennsylvania and Pennsylvania Hospital, working with colleagues to address the diverse needs of his patients. He notes that the comprehensive and collaborative care offered by Penn was part of the appeal of joining the faculty here.
“For patients with head and neck cancer, the part of the body that is affected, our face and head, is not only part of our identity, but it has significant functions,” Shanti says. “Penn’s Abramson Cancer Center, of which the faculty of Penn Dental’s Department of Oral and Maxillofacial Surgery are part, brings all the specialists together to get these patients back to their day-to-day. Our team includes surgeons, radiation oncologists, medical oncologists, nurse navigators, speech language pathologists, nutritionists, social workers, oral-medicine specialists, prosthodontists, and we all go over each case together. It’s patient-centered rather than practitioner-centered.”
Shanti has seen a lot of progress in his field. Today, he’s able to plan out surgeries thoroughly in advance using digital tools.
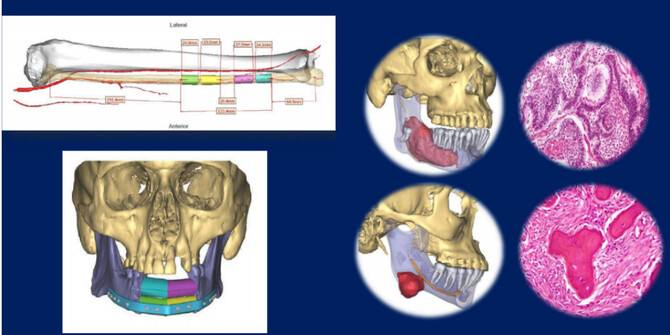
“I can get on a computer with images of the patient, design the surgery, simulate it and identify where I’m going to make the cuts in bone, how the tumor is going to come out and how I’m going to rebuild it,” he says. “Then I’m provided with customized materials, cutting guides and plates designed specifically for the patient. It not only helps increase the precision and accuracy of the surgery, but it also minimizes the time we spend in the operating room because we’re not doing that guess work that’s already done.”
Still he feels there is a long way to go.
Describing another case, Shanti this time shows a photo of a bright, healthy-looking smile.
“This is from a patient I saw Monday,” he says. “She had an ameloblastoma and we did a computer planned and customized free-flap reconstruction using bone and skin from her lower leg. She has a dental prosthesis and is doing well.”
Shanti hopes it won’t be long before many more patients will be able to arrive at this stage, with fewer invasive procedures.